It has been widely known for many years that stomach ulcers are a significant cause of poor performance in sport horses. More recently, it has been discovered that they can be found throughout the equine world and also cause other nonspecific symptoms. Horses that are under many varied types and degrees of stress may develop gastric ulcers.
Signs may include:
- recurrent colic
- change in attitude/behavior
- weight loss/ poor hair coat
- teeth grinding
- inappetence (food and/or water)
- sensitivity to touch around abdomen/flanks
These symptoms are very non-specific.
Unfortunately, the only way to diagnose these ulcers is by direct visualization with a flexible fiber-optic scope: a gastroscope.

At BVS, we have a portable 3.0 meter gastroscope that allows us to examine the entire stomach, as well as a short portion of the duodenum (beginning of the small intestine). Horses are required to be off food for 14-16 hours (they can have water, but this should be pulled 2 hours prior to the appointment) to allow unobstructed viewing. Generally the horse is sedated, the gastroscope is passed through the nostril into the stomach (just like a nasogastric intubation) and the process is completed in less than an hour in your own barn. Problem cases can be fasted overnight in our clinic and scoped there.
All of the pictures below were taken at our clinic, during a normal gastroscopic exam.
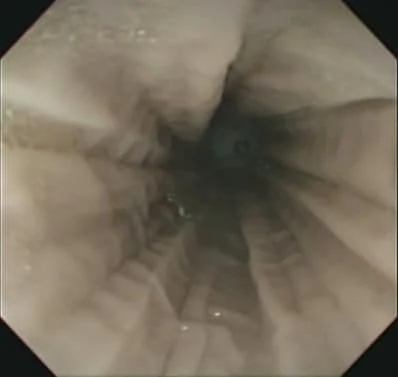
As we enter the esophagus, the normal longitudinal folds, saliva, and peristaltic movement can be seen.
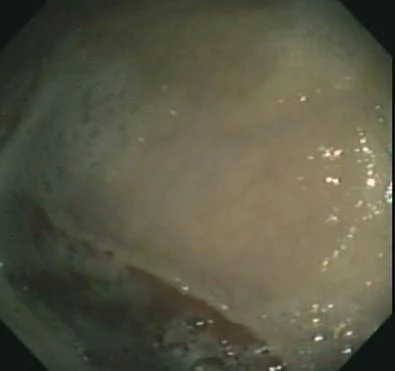
In the body of the stomach, or "fundus", we see two types of tissue. The non-glandular portion is pale, and the glandular portion is darker. The line that divides the two is called the "margoplicatus". Frequently, ulcers are found just above this line.
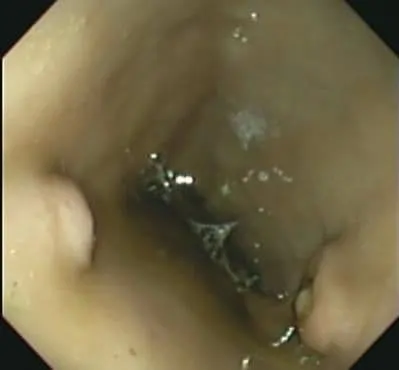
After examining the fundus, the scope follows the "greater curvature" of the stomach, and usually passes through some stomach fluid on the way to the pylorus. Once through to the pylorus (the exit), we see the typical tan-grey appearance of the proximal duodenum (small intestine). Green bile will be typically be found here, and the opening to the bile ducts can be seen. The "bumps" seen below are the openings to the bile ducts.
Now for the abnormal (ulcerated) stomach images...
This is a Grade 1 ulcer: the glandular tissue appears thinner than normal, and the pink area is inflamed.
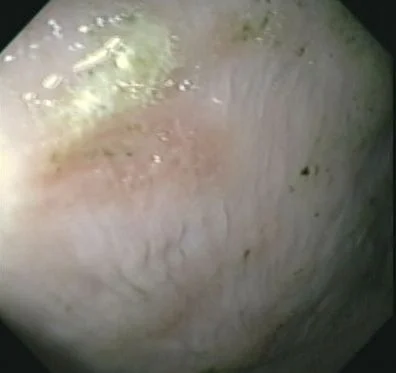
Here again is the pale, nonglandular portion of the fundus with pitted, red ulcerations in the most common place to find them: just above the margoplicatus. (Seen at bottom left). More dramatically, we occasionally find bots, which are parasites that live in the stomach. These are easily taken care of with ivermectin.
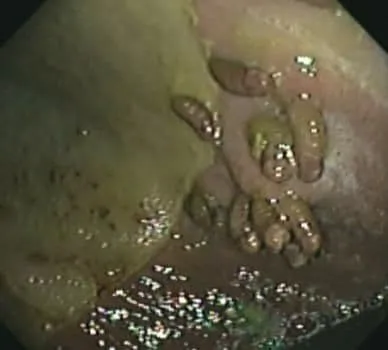
These are more dramatic abnormalities affecting the same region. Many scattered angry red lesions are seen across the mucosal surface. The normal tissue has been eaten away leaving small craters. The margoplicatus is seen at the bottom right of the picture.
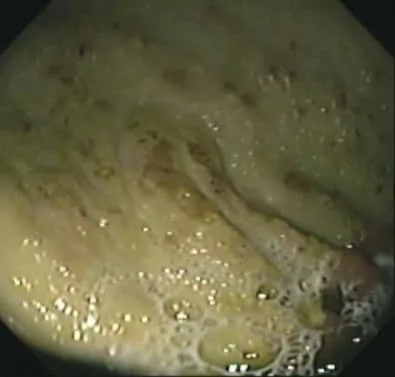
This is a much more aggressive lesion, with the superficial layers destroyed and an open, red lesion showing. This is a Category 3 ulceration.
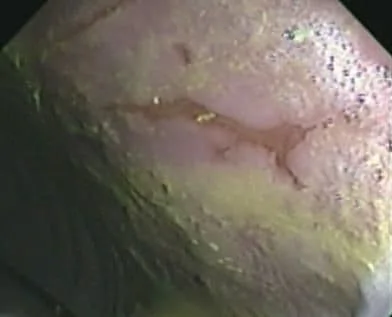
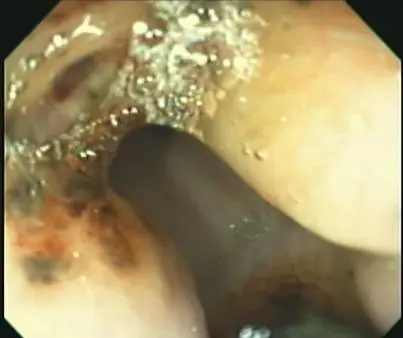
Moving past the stomach fluid and entering the pylorus, we can see the red and dark mottled areas typically seen as ulcers here. These sometimes appear to be weeping serum. Treatment may include an antibiotic and sucralfate as well as Gastrogard specifically for these lesions.
TREATMENT AND PREVENTION
Usually 28 days of a full tube of Gastrogard (omeprazole, dosed by weight) is enough to "cure" these ulcers. Environmental changes are also very important as ulcers tend to re-occur. Feed hay before concentrate (grain) to buffer the stomach acid, especially alfalfa hay that has Calcium and Phosphorus. A lower starch diet, a slow feeder hay net (to keep them eating all day long), and avoiding Bute and Banamine (which can cause stomach ulcers) are all important to help prevent recurrence. Before stressful events, like trailering, showing, etc., it's recommended to use 1/2 tube of Gastrogard once a day starting two days before, and extending through the event.
Gastrogard and Ulcergard are the same product, in the same concentration. They are labeled differently, but can be used interchangeably.